What Is Dysphagia?
“Dysphagia” dys-pha-gia/ (-fa’jah) is defined as a difficulty or discomfort in swallowing, as a symptom of a disease and can include deficits involving the oral cavity, pharynx, esophagus, and gastroesophageal junction.
Complications resulting from dysphagia can include malnutrition, dehydration, aspiration, aspiration pneumonia, chronic lung disease, and even death.
All age groups are affected by dysphagia and its true prevalence is often underestimated as many are undiagnosed.
ASHA provides statistics from multiple sources.
Conservative estimates suggest that dysphagia may be as high as 22% in adults over 50 years of age. [1]
As high as 30% in elderly populations receiving inpatient medical treatment [2] up to 68% for residents in long-term care settings [3]
13%–38% among elderly individuals who are living independently [4]
Additional studies suggest that elderly populations have an increased risk for developing dysphagia-related complications such as pulmonary aspiration [5]
A report by the Agency for Health Care Policy and Research (AHCPR; now the Agency for Healthcare Research and Quality [AHRQ]) estimates that approximately one third of patients with dysphagia develop pneumonia and that 60,000 individuals die each year from such complications (AHCPR, 1999).
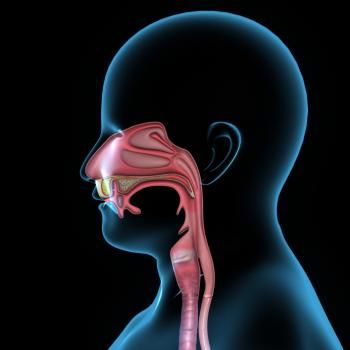
There are 3 phases of swallowing:
- Phase 1: Oral phase in which food is manipulated and prepared to be swallowed.
- Phase 2: Pharyngeal phase in which food must pass from the mouth to the esophagus while being safely directed away from the airway.
- Phase 3: Esophageal phase in which food passes through the esophagus to the stomach.
Difficulties can occur during any of these phases and can range from a mild sensation of food feeling “stuck” in the throat to aspiration, in which food or liquids enter the airway.
What are common symptoms of Dysphagia?
Symptoms can include:
- Drooling and poor oral management
- Food or liquid remaining in the oral cavity after the swallow
- Inability to maintain lip closure, leading to food and/or liquids leaking from the oral cavity
- Food and/or liquids leaking from the nasal cavity
- Complaints of food "sticking" in the oral cavity or throat
- Globus sensation or complaints of feeling an uncomfortable "fullness" in the neck
- Complaints of pain when swallowing
- Wet or gurgly sounding voice during or after eating or drinking
- Coughing during or right after eating or drinking
- Difficulty coordinating breathing and swallowing
- Recurring aspiration pneumonia/respiratory infections and/or fevers
- Extra effort or time needed to chew or swallow
- Changes in eating habits—specifically, avoidance of certain foods/drinks
- Weight loss or dehydration from not being able to eat enough
What causes dysphagia?
Dysphagia results from numerous etiologies secondary to damage to the central nervous system (CNS) and/or cranial nerves, and unilateral cortical and subcortical lesions, due to
- Stroke
- Traumatic brain injury
- Spinal cord injury
- Dementia
- Parkinson's disease
- Multiple sclerosis
- ALS (or Lou Gehrig's disease)
- Muscular dystrophy
- Developmental disabilities in an adult population (i.e., cerebral palsy)
- Post-polio syndrome
- Myasthenia gravis
Dysphagia may also occur from problems affecting the head, neck, and respiratory systems or from general medical complications, including
- Cancer in the oral cavity, pharynx, nasopharynx, or esophagus
- Chemoradiation for head and neck cancer treatment
- Trauma or surgery involving the head and neck
- Decayed or missing teeth
- Critical care that may have included oral intubation and/or tracheostomy;
- Certain medications
- In patients with certain metabolic disturbances
- In patients with infectious diseases (e.g., sepsis, acquired immune deficiency syndrome [AIDS])
- In patients with a variety of pulmonary diseases (e.g., chronic obstructive pulmonary disease [COPD])
- In patients with Patients with gastroesophageal reflux disease [GERD]
- In patients following cardiothoracic surgery
- In decompensated elderly patients
How can Dysphagia be treated?
The primary goals of dysphagia intervention include
- Safely supporting adequate nutrition and hydration and return to safe and efficient oral intake (including incorporating the patient's dietary preferences and consulting with family members/caregivers to ensure that the patient's daily living activities are being considered)
- Determining the optimum feeding methods/technique to maximize swallowing safety and feeding efficiency
- Minimizing the risk of pulmonary complications
- Reducing patient and caregiver burden while maximizing the patient's quality of life
- Developing treatment plans to improve safety and efficiency of the swallow
Therapy techniques can include
- Biofeedback
- Diet modifications
- Electrical stimulation
- Compensatory maneuvers
- Oral and pharyngeal range of motion and strengthening tasks
- Pacing and feeding strategies
- Postural/position techniques
- Prosthetics/appliances
- Medical management
What is a FEES exam?
Fiberoptic/Flexible Endoscopic Evaluation of Swallowing (FEES) is a procedure that can be preformed in a clinical setting or at beside. It is an instrumental diagnostic evaluation which utilizes modern technology to evaluate and manage swallowing difficulties. The procedure uses a flexible fiberoptic laryngoscope which is passed transnasally (slides in along the floor of the nose) to the hypopharynx (the back of the throat). At this point, the larynx and the surrounding structures can be viewed. The scope sits high in the throat, and does not pass between the vocal folds. Colored foods and liquids are given to the patient, and the swallow function is viewed. A FEES allows the Speech-Language Pathologist to not only determine if deficits exist, but also to assess effective therapeutic or positioning strategies and to develop effective treatment plans designed to optimize a patient's quality of life and safety with an oral diet.
Treating therapists use the results of the FEES to determine effective ways to rehabilitate or compensate for the swallow deficits as well as to determine the safety for diet texture and liquid viscosity upgrades.
Sources:
References:
- [1] Lindgren & Janzon, 1991; National Foundation of Swallowing Disorders, n.d.; Tibbling & Gustafsson, 1991
- [2]: Layne, Losinski, Zenner, & Ament, 1989
- [3] National Institute on Deafness and Other Communication Disorders [NIDCD], n.d.; Steele, Greenwood, Ens, Robertson, & Seidman-Carlson, 1997
- [4] Kawashima, Motohashi, & Fujishima, 2004; Serra-Prat et al., 2011
- [5] Altman, Yu, & Schaefer, 2010; Marik, 2001; Schmidt, Holas, Halvorson, & Reding, 1994; Tracy et al., 1989
